At ECCO 2020, IBDoc® was again under the spotlight as 2 very interesting posters were presented. After 5 years of market presence, long term data about the impact of IBDoc® usage in clinical routine are beginning to emerge. Improving quality of life of IBD patients is extremely important, developing tools to allow patients to have a higher sense of control over their disease is now a must, especially for chronic diseases. Kathleen Sugrue assessed this in her poster at ECCO 2020.

By loading the video, you agree to YouTube's privacy policy.
Learn more
At Mercy University Hospital, the goal of the study was to assess the impact of IBDoc® in clinical practice. Since 2014, 733 patients were enrolled in the IBDoc® program. The clinic now has sufficient experience with this tool to allow an evaluation. The patients were allowed to stay at home and came to the hospital for further evaluation only if the IBDoc® result was elevated (>100µg/g). Over the last 6 months, a total of 240 tests were performed by patients. Of those, 40% were normal, 40% were moderate and 20% were high. Only the patients with a moderate or a high result were scheduled for an appointment at the hospital within a week. Of the moderate, 20% had a change of therapy and of the high results, all patients were booked for an urgent colonoscopy and all were found to have an active disease.
This study has several outcomes. First of all, the IBDoc® set-up allows to free-up time both on the patient side, who is no longer coming to the hospital, and on the hospital side, where the care givers could now focus more on patients with active diseases. The patients are only coming to the clinic when it is needed, enhancing the patients quality of life. Next, we can see that IBDoc® has a 100% correlation with endoscopy, which makes it an excellent tool for patient monitoring and allows the fast track system in clinical practice.
On the same topic, an internal audit was conducted at Dorset County Hospital to evaluate the efficiency of IBDoc®, which is used there since 2016. Pearl Avery presented the audit findings in her ECCO 2020 poster to better assess the benefit for patients and hospitals. The study is a retrospective evaluation of the most recent results generated with IBDoc®. Correlation between fecal calprotectin and endoscopy or patient disease state was then evaluated.

By loading the video, you agree to YouTube's privacy policy.
Learn more
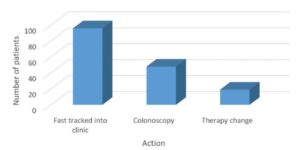
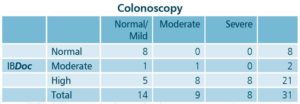
Over the last 6 months, 134 patients were registered to use IBDoc®. Of those, 111 patients generated a result. Based on this result, 31 patients were scheduled for a colonoscopy and an 84% correlation between fecal calprotectin and colonoscopy was found. It is important to note that, for high results generated with IBDoc®, correlation goes up to 100%. In patients having normal colonoscopy result but a high calprotectin value, other reasons for the high calprotectin was found, such as C.difficile infections and others. Of the 80 patients with no colonoscopy, disease status was assessed and 39 patients were deemed well, 19 needed a tighter monitoring and 23 needed a change of therapy. These outcomes correlate very well with IBDoc® thresholds: Normal (<150), Moderate (150-400) and High (>400).
As for the first poster, the aim was here to demonstrate the good correlation between IBDoc® and endoscopy. This allows to better identify the patients in need for further evaluation and those who don’t, increasing time management for both the clinic and the patient.